Patterns in women’s health: Gynaecological and Gastrointestinal comorbidity
04/06/2021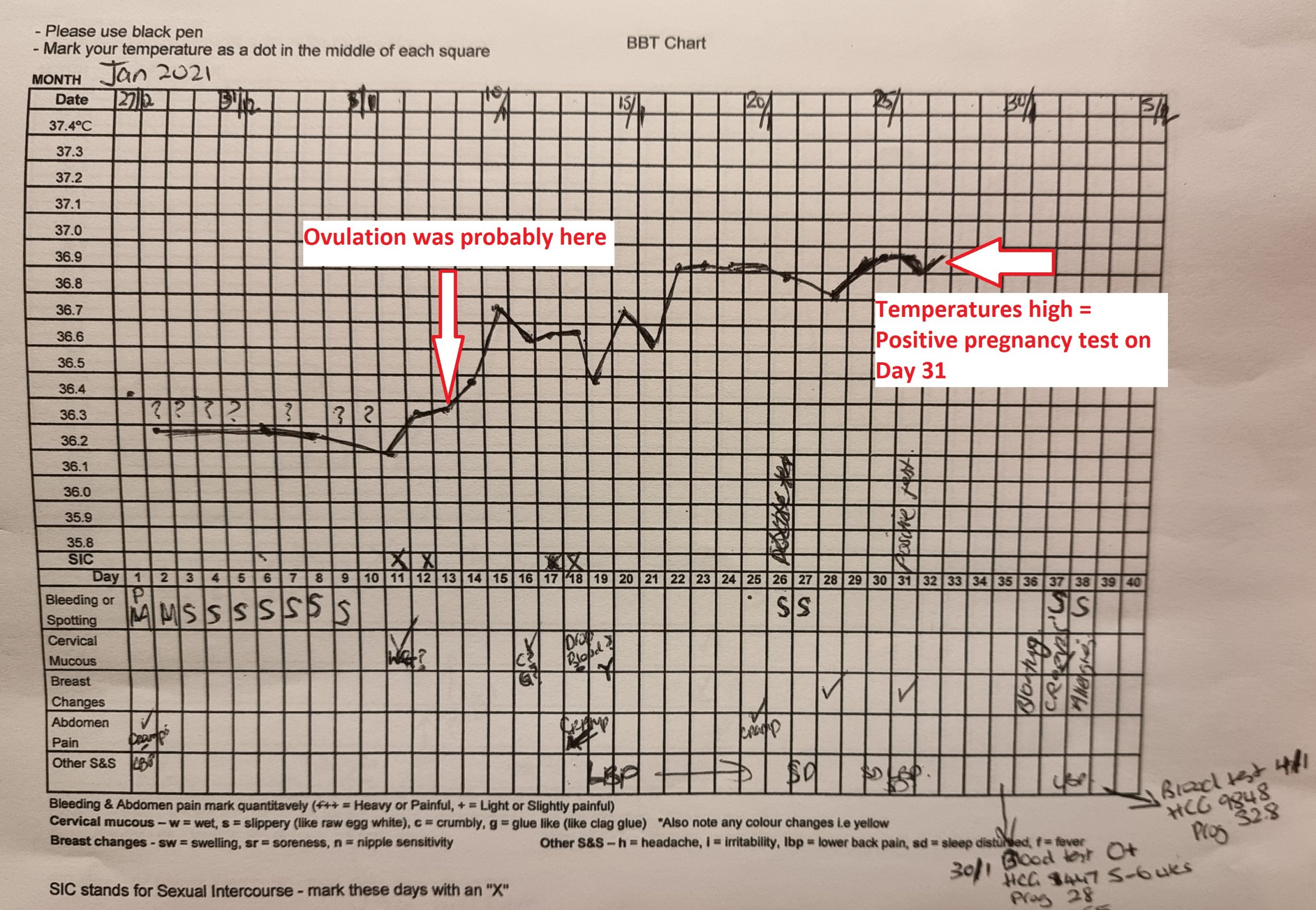
How to use a BBT chart to help you fall pregnant
05/08/2021
How Traditional Chinese Medicine treats PCOS
Diagnosis in Chinese Medicine
We are frequently asked by very well-meaning, curious people, questions like
“Can Chinese Medicine treat endometriosis?”
“My sister keeps having miscarriages, can you help?”
“What can you do for PCOS?”
The answer unfortunately isn’t black and white, it’s not as simple as saying “yes” or “no”. Yet Chinese medicine can always provide benefit in some way, but these questions require a fairly long answer to do it proper justice and to show respect to the person asking.
You see, whilst in Western medicine an absence of disease is classified as health, in Chinese medicine there is a clear difference between someone having health, and someone having vitality.
A better way to describe how Chinese medicine can help someone is that Chinese medicine treats the person, not the disease.
And by “treating the person”, what we actually mean is that Chinese medicine treats the person’s pattern presentation. This however takes a diagnosis, and diagnosing in Chinese medicine is unique. We don’t rely on blood tests, scans and other pathology reports. Most of the time, our patients who see us are “within the normal range” for everything, and their scans are “fine”. Yet they still seek treatment because they know intuitively things are not quite right. Irregular cycles, irregular bowel habits, skin breakouts, recurrent miscarriage etc
In Chinese Medicine, diagnosis is based on observations.
We learn to observe everything.
We use the five senses of looking, touching, listening, asking and smelling in our diagnosis.
We also observe the seasons and the weather and how appropriately the patient interacts with these external elements
Sometimes our diagnosis can begin without the patient even realising. We observe things like how they enter the clinic (rushed, loud, clanging and banging or soft, mindful, respectful), how they sit or stand up from the chair, how they walk.
We listen not only to the main reason that brought the patient to our clinic, and listen as they answer all of our questions, but we also observe the manner in which they speak. The words they use, and the timbre of their voice reveal a lot about how to help them. Some patients sigh a lot, some might clear their throat repeatedly, or sniff, or fidget and these are such ingrained habits that the patient is not usually aware they do it.
These little habits are interesting to observe.
Touching – putting physical hands on the patient reveals more depth to our pattern differentiation. We might feel their pulse and observe is it strong or weak? Is one side stronger than the other. Does it feel tight or wiry? Soggy or slippery? We feel the channels, or parts of the body we want to needle or moxa, and we might notice areas that are taught and tense, gristly and gravelly, or soft and empty.
We look at the tongue and observe its colour, coat, and body shape. (For more about the tongue, please read this blog post.) We look and observe skin texture and sheen, facial breakouts and where on the face they occur (different aspects of the face relate to different organ systems and help refine diagnosis) facial expressions, overall body language and body shape.
Smelling as part of diagnosis is not done in an obvious manner. For example, we don’t ask “Can I smell your armpits?” (Because that would be NOT GREAT!)….however we will make a mental note if there is frequently bad breath (digestive health isn’t optimal), or other odours that in our textbooks are described as “damp/musty, burnt, sweet” etc Different smells correlate with different organ and pattern pathology in Chinese medicine.
In essence, our methods of diagnosis are at the same time both obvious and subtle. We use these methods to try and explain what pattern the patient is displaying. Is Qi stuck? Is Qi depleted? Is there cold, heat or dampness? Where is it? How did it get there? How can we, the practitioner, help to regulate this? But more importantly, what is the patient doing that regularly contributes to this and how can they change to help facilitate faster healing?
So when asked,, “What can you do for PCOS?”
The answer is complex.
Just like two snowflakes are never identical,or the pattern on leaves are never quite the same. No two cases of PCOS, or endometriosis, or recurrent miscarriage are ever the same.
Women with PCOS for example, all have similarities. They all have PCOS. They might all have bad skin and have difficulty losing weight.
But some have a heavy period. Some have a light one. Some get two periods a year while others have a period every 40-50 days.
Some have period pain, others don’t.
Some PCOS patients don’t have any issues with their weight.
Some have always had irregular cycles, and some only experience it after coming off contraception.
Some women have frequent headaches, whilst others have sleeping issues. Some feel hot all the time, whilst others always have cold hands and feet.
It is the finer nuances that enable a Chinese medicine practitioner to diagnose and differentiate patterns. The practitioner chooses acupuncture points and Chinese herbs according to what they deduce the pattern is. Advice on lifestyle or diet is given based on these same principles. Every single person has a unique pattern and this pattern will change as they move towards healing.
We don’t treat the PCOS.
In Chinese medicine we treat the person and their pattern, not the disease.