Melatonin and fertility
16/05/2019
When you’re cold, you’re dead.
27/01/2020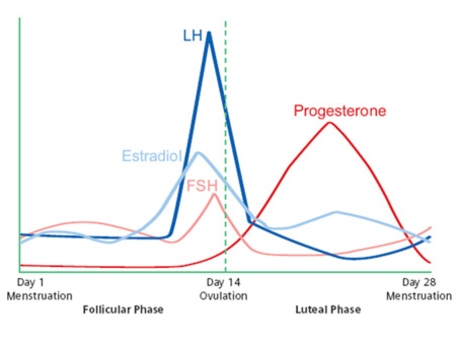
What do my hormones do throughout my cycle?
In clinic, we frequently encounter women who want to fall pregnant but have absolutely no idea about their bodies and their cycles.
It is SO COMMON!
Some don’t even know when to start counting day 1 of their cycle (hint: it’s the first day of your period/bleeding, not the last).
We believe it’s important for all women to understand how, and what, their body is doing.
We are often explaining the ins and outs of hormones throughout the menstrual cycle during a consult – the names of the hormones involved, what the different phases are, how to predict ovulation etc
It’s the stuff that should have been taught in High school pd/h/pe classes. But instead we’re taught how not to fall pregnant! (I get it, safe sex is important, but at the same time, we need to be unravelling all the misconceptions of periods and cycles and de-stigmatising a woman’s body).
Some terms that will be used in this blog post are:
FSH: Follicle Stimulating Hormone
LH: Luteinising Hormone
Oestradiol: the main type of oestrogen found in women
Progesterone: a hormone that supports the early stage of pregnancy
Chances are, if you’ve been trying to fall pregnant, you would have heard about these hormones, but you’re probably unclear about how they work, when they work or what they do.
So let’s explain your cycle in a no nonsense easy to understand way!
There are essentially 2 “phases” to your menstrual cycle, the Follicular phase and the Luteal phase.
What is the Follicular phase?
The follicular phase is counted from the first day or your period to the day that you ovulate.
It is called the follicular phase because it is influenced mostly by Follicle Stimulating Hormone (FSH).
Good to know:
Your ovulation day may, or may not be, day 14 of your cycle.
You count Day 1 of your cycle as the first day of bleeding, not your last. Ovulation is not determined by when your period finishes.
Your Follicular phase can vary in length from cycle to cycle and it most definitely can vary from woman to woman. Not all of us have a “perfect” 28 day cycle.
Follicles are not eggs
Really simply:
A gland in your brain (the pituitary gland) produces Follicle Stimulating Hormone (FSH). FSH is carried by your blood to your ovaries. FSH stimulates follicles to grow. Follicles start growing from Day 1 of your cycle. We have found no agreement in articles and texts on what is considered a “normal” amount of follicle growth, but it seems that “roughly” between 6-15 follicles is normal. Normally, follicles will grow on both ovaries, with one side growing more than the other. As you approach ovulation, one of these follicles will start growing bigger and faster than all the others. It’s known as the dominant follicle. It is this follicle that contains the mature egg that will be released when you ovulate.
Ovulation and the LH surge
Ovulation is a process determined by a fine balance of hormone exchange. While FSH is encouraging lots of follicles to grow, LH, luteinising hormone, is also produced in small amounts (by the same gland in the brain that produces FSH, the pituitary gland) throughout the follicular phase. LH encourages the follicles already growing to produce oestradiol (oestrogen).
As you approach ovulation, a surge in LH will help to ripen the dominant follicle and rupture it for the egg to be released.
This surge is what the ovulation test kits try and pick up on. You can find out more about ovulation and how not to rely on ovulation kits in our blog post about fertile mucous.
Our opinion on Ovulation kits:
We are not the greatest fans of these kits for a number of reasons. They are not entirely accurate – they are testing LH, which is always in your system, just in varying amounts. (Unlike a pregnancy test which tests for a specific hormone – HCG – which is only in your system if you are pregnant). The ovulation test tries to predict a surge, but you don’t know where you are in that surge when you test. You might miss your ovulation while you wait to pick up on the LH surge. And for a test that is hard to read, and not 100% accurate, they are hideously expensive. For some women, if your waiting for the test to “tell” you your ovulating, sometimes that’s too late to start having sex. Please read more about mucous and how to tell your fertile mucous, on our “What is fertile mucous” blog post.
Interesting facts:
Your fallopian tube is not attached to the ovary. The end of the tube has tiny “fingers”, technically called fimbriae, which are constantly swaying and moving in fluid (much like seaweed), creating currents which “sweep” the released egg into the tube.
If the egg is fertilised but gets swept outside of the tube, rather than inside, and implants outside, this is how ectopic pregnancy develops.
What is the Luteal phase?
The luteal phase is counted from your day of ovulation to the day just before your period. A normal luteal length is generally between 12-14 days
It is called the luteal phase because Luteinising hormone (LH) is the most influential hormone.
After ovulation, the ruptured follicle is now called the corpus luteum. LH stimulates the corpus luteum to produce progesterone which helps to support the early stages of pregnancy. The corpus luteum produces both progesterone and oestradiol and the primary role of these two hormones is to ensure that the lining of the uterus is fully prepared for implantation, if fertilisation occurs. If you are not pregnant, towards the end of the cycle the corpus luteum breaks down, progesterone production decreases and the next menstrual cycle begins when follicle stimulating hormone starts to rise again.

I hope this has clarified some terms for you (and I really hope I haven’t confused you!). Discussing the menstrual cycle and all the hormones involved is an intricate and complicated process. If you want to find out more about your cycle please phone us to make an appointment! We’d love to help you!